STIs - Sexually Transmitted Infections
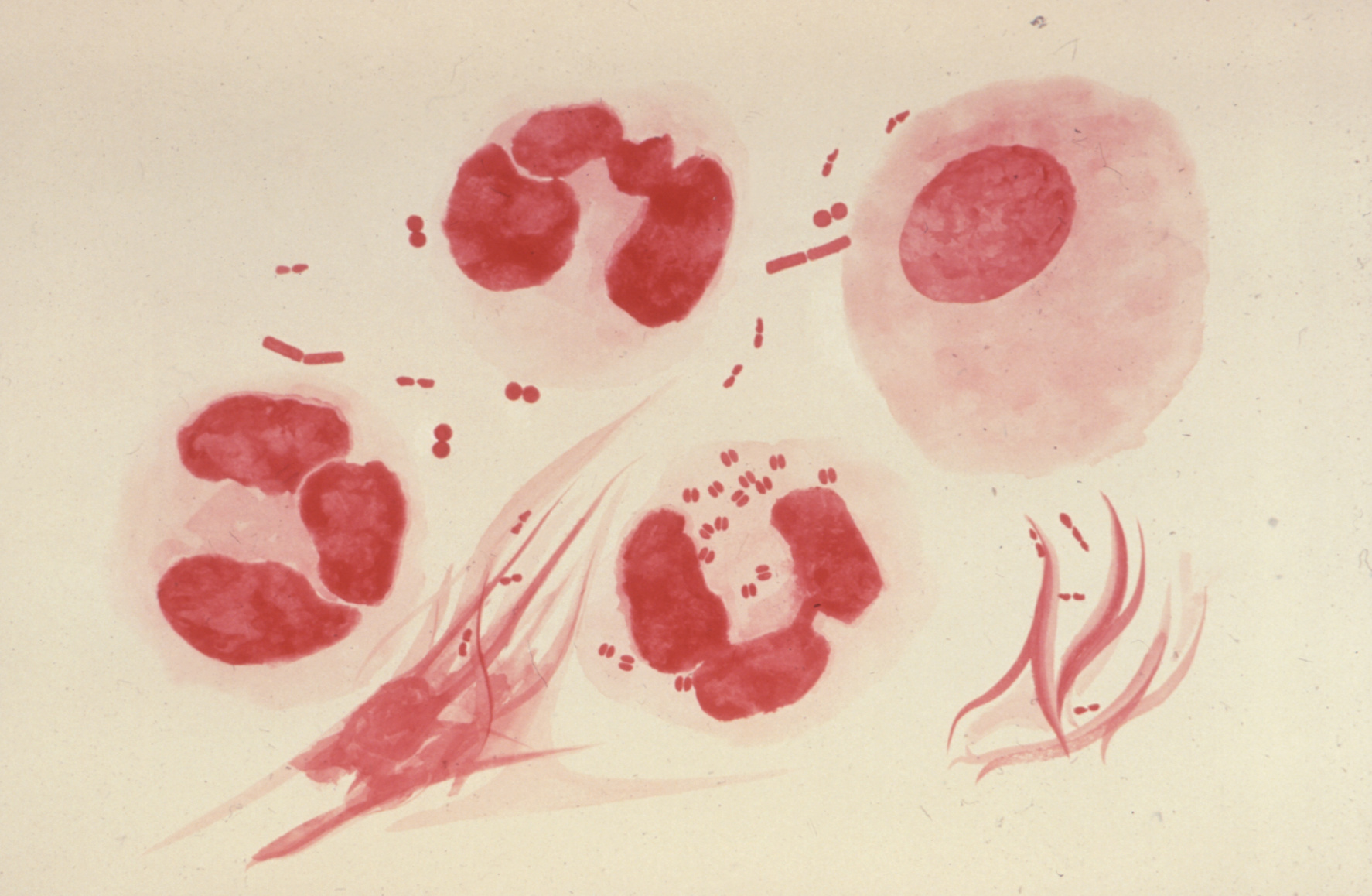
STIs or Sexually Transmitted Infections are diseases that are passed from one person to another through unprotected sex or in some cases through genital contact. Most STIs such as Chlamydia often don’t show signs of infections at all, which makes the spread of the diseases hard to stop. One in twelve people tested in the UK has an infection, which can lead to infertility. The most common STIs are Chlamydia, Gonorrhoea, Syphilis caused by different bacteria; Genital Herpes, Human papilloma virus and AIDS caused by viruses; and Trichomoniasis caused by a parasite. (1)
But humans are not the only animals suffering from STIs, all other animals can be infected by diseases transmitted during sex.
The STI comeback: the infectious social apps
STI in animals
What animals tell us about STIs
Finding vaccines
Animal research leading to therapeutic drugs
The STI comeback: the infectious social apps
STI were thought to have been increasingly under control with decreasing infection rates (2) but in recent years they are making a significant comeback, which some scientists are correlating to the rise of dating applications (apps). Match making apps such as Tinder have accumulated 50 million users since 2012 and now match 15 million people a day while Grinder, focussing on homosexual men, has 6 million users making 10,000 matches a day. Finding a sexual partner has never been faster and easier.
Syphilis was almost on the brink of extinction in the US and UK at the end of the last century thanks to penicillin but it has made a huge comeback with the UK now reporting 3,000 cases a year and the US 16,500. Studies show that dating apps are a ‘hyper-efficient mean of transmission’. (2)
App users are more likely to sleep around and have already had an STI. Men who use apps to find partners are 40% more likely to test positive for gonorrhoea for example. Online interactions also increase risk taking and join together previously isolated sexual networks within which diseases had been previously contained, disseminating the STIs even more.
Of course, dating apps are not the only ones responsible, the rise in Syphilis in the UK and US for example also correlates with a reduction in sexual health campaigns and a change in attitude towards AIDS, a disease that is no longer life threatening, at least when modern medicines are available. (2)
STIs in animals
“Wild Animals don’t practice safe sex, of course they have STIs!” explains Dr Barbara Natterson-Horowitz, a modern day Dr Dolittle and UCLA cardiologist consulting for the Los Angeles zoo. Atlantic bottlenose dolphins can get genital warts, baboons suffer from herpes and syphilis is common in rabbits. (3)
STIs in animals and humans have a historical relationship. “Animals suffer from almost all of the diseases that human beings do but veterinarians and physicians never talk about this. Physicians have not traditionally seen veterinarians as their clinical peers and that is unfortunate”. (3) Indeed, studying STIs in both humans and animal could save lives for both. “Two or three of the major STIs [in humans may even] have come from animals” says Alonso Aguire, a vet and president for conservation medicine at wildlife trust” (4).
“We know, for example, that gonorrhoea came from cattle to humans. Syphilis also came to humans from cattle or sheep many centuries ago, possibly sexually”. The most recent and deadliest STI to have crossed the barrier separating humans and animals has been HIV, which humans got from the simian version of the virus in chimpanzees.
The most common STI among animals today is Brucellosis or undulant fever present in domestic livestock, dogs, cats, deer and rats. It is also transferable to humans by drinking contaminated milk or direct contact with the infected animals and can be very dangerous to humans, one reason why milk is pasteurised.
Overall, Humans STIs have enough in common with animal STIs that much can be learnt about human STIs by studying them in animal models. (4)
What animals tell us about STIs
The study of STIs in animals can tell us a lot about their pathogenicity. Lockhart and Thrall (5) studied 200 diseases with evidence of sexual transmission in mammals, reptiles, arachnids, insects, molluscs and nematodes. These pathogens included protozoans, fungi, nematodes, helminths, cancerous cells, bacteria and viruses.
They found that the dynamic of STIs differ from infectious diseases in that it depends on frequency or proportion of infected host in the population rather than on host density, which correlates with other studies pursued on the ladybug and theoretical models of host-STI systems. (6) Their study also highlights that STIs cause less mortality and are longer lived than their hosts, are less likely to invoke a strong immune response, have narrower host ranges and show less fluctuation compared to infectious diseases. These shared features are related to their mode of transmission – sexually – rather than their host or pathogen affiliation. The main driving force for their evolution was their ecology and mode of transmission rather that the phylogenic classification of both host and pathogen. (5)
Studying an STI in an animal help us predict its behaviour in humans. For example, animal studies have suggested that the ‘viral reservoir’ in which HIV lies dormant is established much earlier than previously thought (More information of AIDS https://www.animalresearch.info/en/medical-advances/diseases-research/aids-hiv/ ). It is established in tissues in thefirst few days of infection, before the virus can be detected in the blood. Studies of the Rhesus monkey showed that the earlier the antiretroviral treatment started, the longer the virus took to rebound or become detectable in the blood, but was still present. This would explain de the late symptoms of the baby ‘cured’ from HIV last year. This mirrors well the need to continue to study the way STIs function in animal models to fully understand them and find ways to stop them. (7)
Finding vaccines
Animal models are also really important in finding a cure or even better, a vaccine. Research on HIV today is actively looking for a vaccine.
“There is no protective vaccine against HIV today and it is a priority to find one.” states Dr Dr Monsef Benkirane, director of the human genetic CNRS institute in Montpellier and specialist in HIV persistence. “If one day we find a vaccine, it won’t be a classic vaccine like we know them today. It will be profoundly new.” Because HIV infects the immune system, evades it and changes so rapidly, finding a way to vaccinate against it has been particularly challenging - classic antibody vaccines haven’t proven to be efficient enough. (8)
However, important and promising advances have been recently achieved by scientists working at the development of powerful antibodies found in 20% of AIDS patients capable of neutralizing HIV.
“The discovery of broadly neutralising antibodies brings a hope for HIV cure. Indeed, proof of concept of their efficacy using animal models has been recently reported. These antibodies are able to decrease the viral load in chronically infected animal even better than the antiretroviral drugs in use today. Based on results obtained using animal models, clinical trials using this antibody are ongoing.” explains Benkirane. (8)
In Australia a group of researcher is working on a Chlamydia vaccine for Koalas as a step towards a human vaccine. With only 43,000 koalas left in the wild, Chlamydia has greatly contributed to a decrease exceeding 80% of the koala population in the last 10 years in some places. Peter Timms and Ken Beagley, originally working on human Chlamydia before switched to the koala’s version in order to discover an effective vaccine. With still three more trials needed to get the vaccine completed, the team is envisioning the potentials for humans. However, the homology and transferability of the vaccine to humans is difficult to predict, as there is only 10% similarity between the koala and the human Chlamydia. But the goal is to find antigens that are conserved across all Chlamydia species. (4)
Animal research leading to therapeutic drugs
In humans, some STIs can thankfully be cured using antibiotics. But like all drugs, tests on animals are performed before they can be given to humans. These tests help understand the efficacy of the drug, but also the side effects and the dosage. Doxycycline is one of the main antibiotics given to cure Gonorrhoea, syphilis and Chlamydia. Animal studies have shown that the drug can be dangerous for pregnant women and their foetus, as it can cross the placenta, although it doesn’t seem to affect fertility in female rats.
Animal tests have also shown evidence of oncogenic activity and mutagenic effects in rats for some related antimicrobials. For example, the antibiotic-linked hyperpigmentation of the thyroid was studied in minipigs, and dogs.
Animal testing remains crucial for ensuring new drugs are safe for humans. (9)
References
- http://www.stiday.uk/
- http://www.newscientist.com/article/mg22530020.600-a-date-with-disease-get-the-app-risk-the-clap.html
- http://abcnews.go.com/Health/zoobiquity-diseases-animals-share-humans/story?id=16549555
- http://discovermagazine.com/2008/sep/09-how-often-do-animals-get-stds
- http://www.ncbi.nlm.nih.gov/pubmed/8761160
- http://webspace.qmul.ac.uk/rknell/STDs.html
- http://gracepointwellness.org/13-sexually-transmitted-diseases/news/165819-animal-experiments-shed-light-on-hivs-ability-to-hide
- http://www.understandinganimalresearch.org.uk/news/research-medical-benefits/world-aids-day-2014/
- http://www.drugs.com/doxycycline.html
Last edited: 14 January 2015 12:42
