Anthrax
Back in the 19th century, Anthrax was a disease of sheep and cattle that was of enormous importance. Each year 5% of cattle and 10% of sheep died of Anthrax in France. In some particular areas of France and Argentine, the mortality rate of farm animals was so great the land had to be left unused.
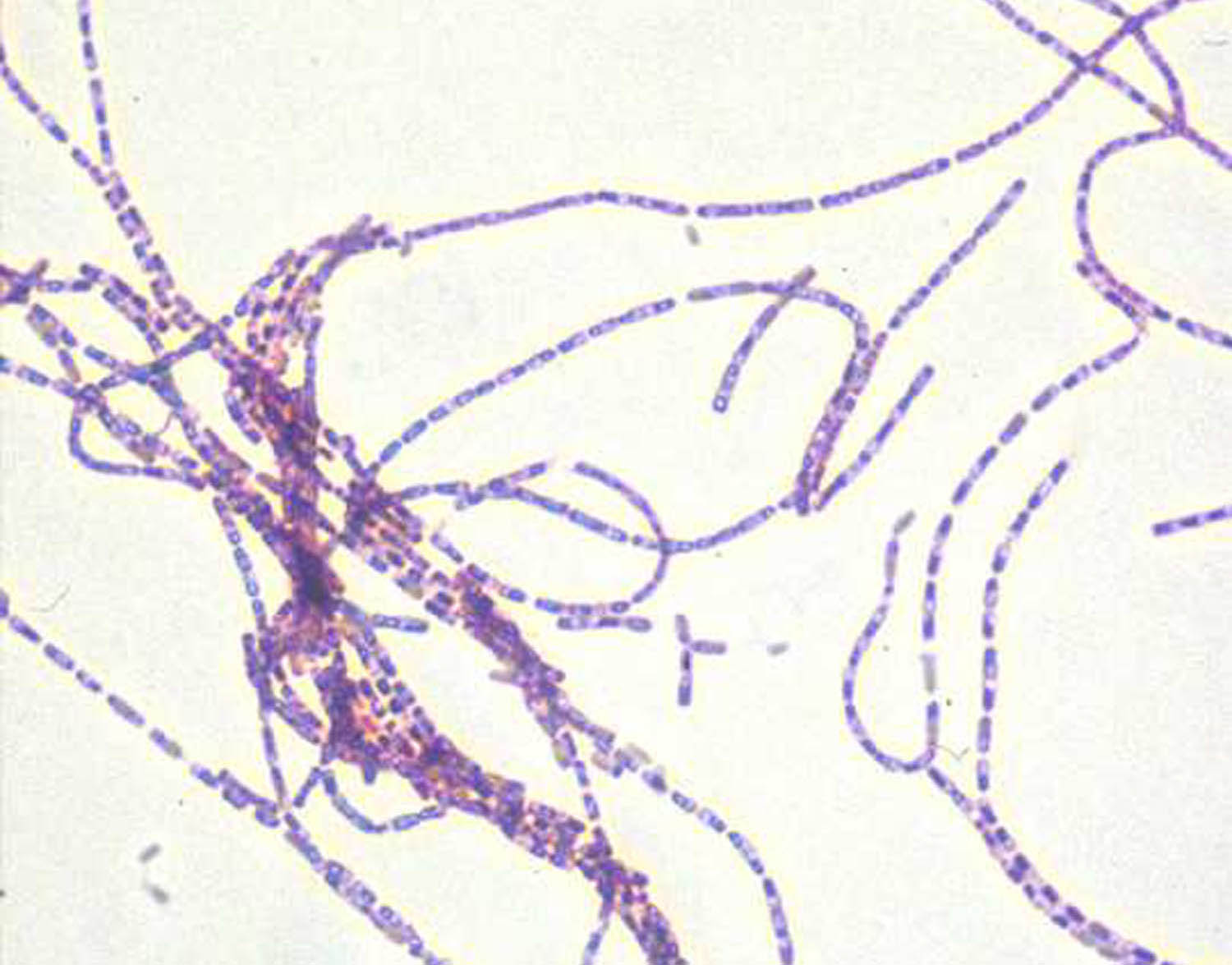
Anthrax is a zoonotic disease caused by a relatively large spore-forming rectangular shaped bacterium called Bacillus anthracis. It mostly spreads in wild and domestic herbivores but can occasionally affect humans exposed to infected animal tissue or products. It does not typically spread from animal to animal nor from person to person. The bacteria produce spores on contact with oxygen.
In herbivores, the anthrax bacterium produce extremely potent toxins which commonly presents as an acute septicaemia with a high fatality rate, often accompanied by haemorrhagic lymphadenitis. In dogs, humans, horses, and pigs, it is usually less acute.
Discovery by Pasteur
Pasteur was the first to address the problem of the prevention of the disease. Some bodies, termed bacteridia, had sometimes been detected in the blood of animals suffering from anthrax. Using a culture technique, Pasteur found that the bacteridium would grow freely in neutralised urine.
Convinced the culprit was these small bodies, Pasteur produces successive subcultures diluted from the original virulent culture. Even through the sub-cultures were diluted several million times, upon injection, they could still produce anthrax in guinea pigs. This was proof that the bacteridium was the sole cause of anthrax – everything else had been diluted out.
By a series of experiments, Pasteur then went on to prove that the anthrax bacteridium infected sheep through the alimentary canal. He also explained how the disease persisted in particular ‘cursed’ fields where cattle or sheep were bound to contract anthrax if they grazed there.
Koch had shown that anthrax bacteriadia could form spores in conditions of high oxygen levels and temperature. Pasteur demonstrated the presence of these spores in the fine top soil of the ‘cursed’ fields that could remain infective there for many years.
Earthworms were responsible for bringing up the spores to the surface – sometimes from the buried bodies of anthrax sheep or cattle. The animals then ingested the anthrax spores from grass or clover contaminated by the soil. Pasteur showed that guinea pigs could contract anthrax from extracts of soil even if it was heated to 90°C – which usually kills off other soil bacteria – and from the soil from earthworm intestines.
Making a vaccine
Having already produces a vaccine for chicken cholera, Pasteur sought to develop an attenuated strain of bacteria, in the same way. He looked at the vitality and virulence of cultures treated in various different ways.
The bacteridium grew only between 14 and 44°c, but when cultured towards the higher extremities (42-43°c) a virulent strain grew rapidly but Pasteur found that the virulence waned. These cultures became harmless to guinea pigs after 12 days, but still killed mice. After 4 weeks, even mice and baby guinea pigs survived the heated culture. These surviving animals had gained immunity against anthrax and the varied incubation time allowed Pasteur to make ‘vaccines’ of graded strength.
Pasteur proved the effectiveness of his vaccine with a convincing public demonstration at Pouilly-le-Fort in 1881. Under the supervision of a vet, 25 sheep were inoculated with Pasteur’s vaccine, and 25 were not. All 50 sheep were then injected with a virulent culture of anthrax bacteridia. 3 days later, all vaccinated sheep were healthy while 22 of the non-vaccinated sheep were dead and 3 dying. The same experiment was repeated in 10 cows and was just as successful. For those still in doubt, Pasteur showed the vaccine was also effective when contaminated blood was given to animals instead of cell cultures.
In France, between 1882 and 1893 nearly 4 million animals received the anthrax vaccine, and loss of cattle and sheep from the disease fell to a minimum. The use of Pasteur’s vaccine spread throughout Europe and the World. By 1914, 40 million doses had been sent out from the Pasteur Institute alone.
By a simple animal experiment, of a style and to an extent that could never be reproduced in humans, Pasteur had shown indisputably that immunisation did protect against infective diseases - research that animals themselves benefit from.
Referencias
-
Jack Botting, ed. Regina Botting, Animals and Medicine: The Contribution of Animal Experiments to the Control of Disease. Cambridge, UK: Open Book Publishers, 2015. http://dx.doi.org/10.11647/OBP.0055
-
Descour L (1922) Pasteur and his work. London: T Fisher Unwin
-
http://www.vetmed.wisc.edu/pbs/zoonoses/anthrax/anthraxanimals.html
-
http://www.merckvetmanual.com/mvm/generalized_conditions/anthrax/overview_of_anthrax.html
-
http://www.historylearningsite.co.uk/a-history-of-medicine/louis-pasteur/
Last edited: 19 January 2018 13:58
