Medical discovery timeline
The developments in medicine since the end of the 19th century have been remarkable. It is now almost impossible to imagine a time before it was known how the human body fought the diseases carried by micro-organisms. Since then medical research has transformed healthcare, extending and improving the quality of life for millions. Many of these remarkable discoveries would not have been possible without vital experiments on animals.
-
1881
Germ Theory of Disease

-
1898
Malaria-parasite's life-cycle discovered

-
1902
Mice & genetics

-
1905
Transplant surgery first performed on a human
-
1913
Diphtheria prevented by immunisation

-
1914
Vitamin A discovered

-
1915
Blood transfusion

-
1921
Neurotransmission demonstrated
-
1922
Insulin isolated

-
1926
Pernicious anaemia
-
1937
Heparin used as an anticoagulant
-
1940
Penicillin protects mice against infection

-
1945
Dialysis developed for kidney failure
-
1955
Polio vaccine developed

-
1958
Cardiac pacemakers

-
1961
Artificial heart valves
-
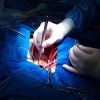
1967
Heart transplants successful in humans
-
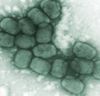
1977
Smallpox eradicated through vaccination
-
1982
Leprosy treatments developed

-
1987
AZT - the first drug treatment for HIV
-
1992
Hib-meningitis vaccine
-
1996
Cloning Dolly the sheep

-
2002
Sequencing & analysis of the mouse genome

-
2012
CRISPR genome editing

-
2021
RNA vaccine against COVID-19
Last edited: 13 June 2023 15:32

